Ten post jest także dostępny w języku:
![]() polski
polski
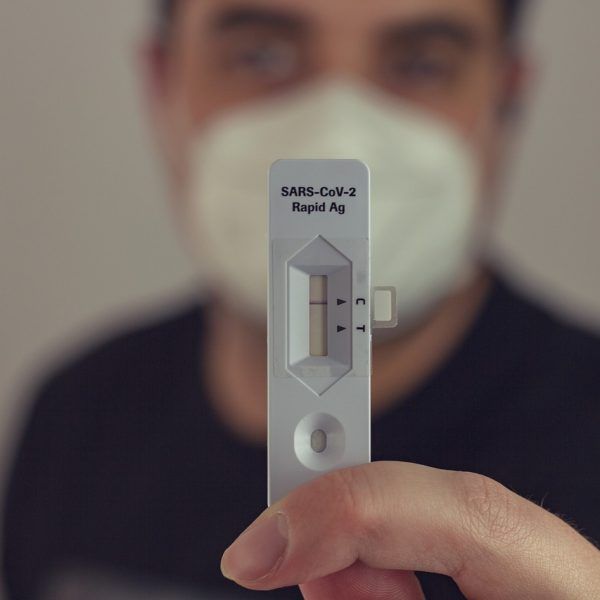
Poland as a leader in the biomedical sector in CEE ?
The COVID-19 pandemic has highlighted the importance of a strong domestic biomedical sector in fostering innovation. Therefore, the government proposed…
Poland as a leader in the biomedical sector in CEE ?
The COVID-19 pandemic has highlighted the importance of a strong domestic biomedical sector in fostering innovation. Therefore, the government proposed…
PMR Exclusive
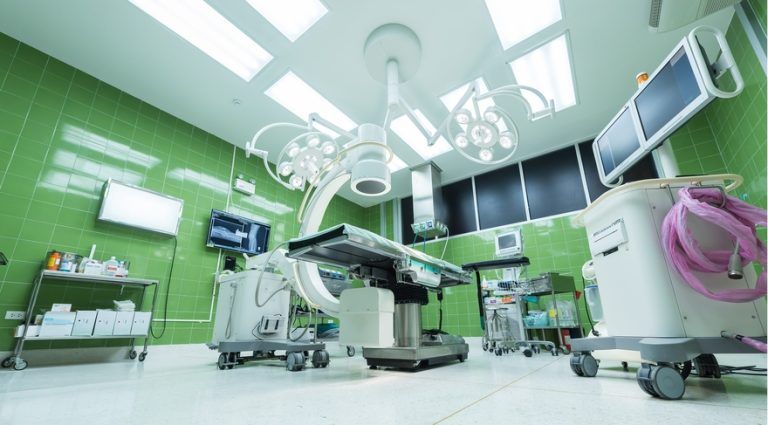
PMR and Upper Finance: significant growth observed in robotic surgery market
Intuitive Surgical, a leading manufacturer of robotic surgery devices, has reported an increase in revenue of 30% year on year…
M&A and investments
Medicover develops Poland’s first eco-friendly dental center
Medicover Stomatologia is expanding the “Rytual Usmiechu” concept, under which numerous dental facilities were opened through the whole 2021. The…
HR changes
Agnieszka Grzybowska-Zalewska appointed as new President of the Management Board of Sanofi
Sanofi-Aventis has appointed Agnieszka Grzybowska-Zalewska to the position of CEO. Previously, since 2013, she served as CEO of Sanofi Genzyme…
Technology
Poland as a leader in the biomedical sector in CEE ?
The COVID-19 pandemic has highlighted the importance of a strong domestic biomedical sector in fostering innovation. Therefore, the government proposed…
Regulations
Poland as a leader in the biomedical sector in CEE ?
The COVID-19 pandemic has highlighted the importance of a strong domestic biomedical sector in fostering innovation. Therefore, the government proposed…